Focus on your patients, not your spending
Is a 5-day AP backlog slowing down critical purchases?
Our 2025 Benchmark Report found that Healthcare Services average 124 hours for AP processing—the slowest across all industries. Unlock 11 key procurement KPIs from $20B+ in spend data—tailored benchmarks for Healthcare so you can identify gaps and optimize faster.

Configurable purchasing workflows
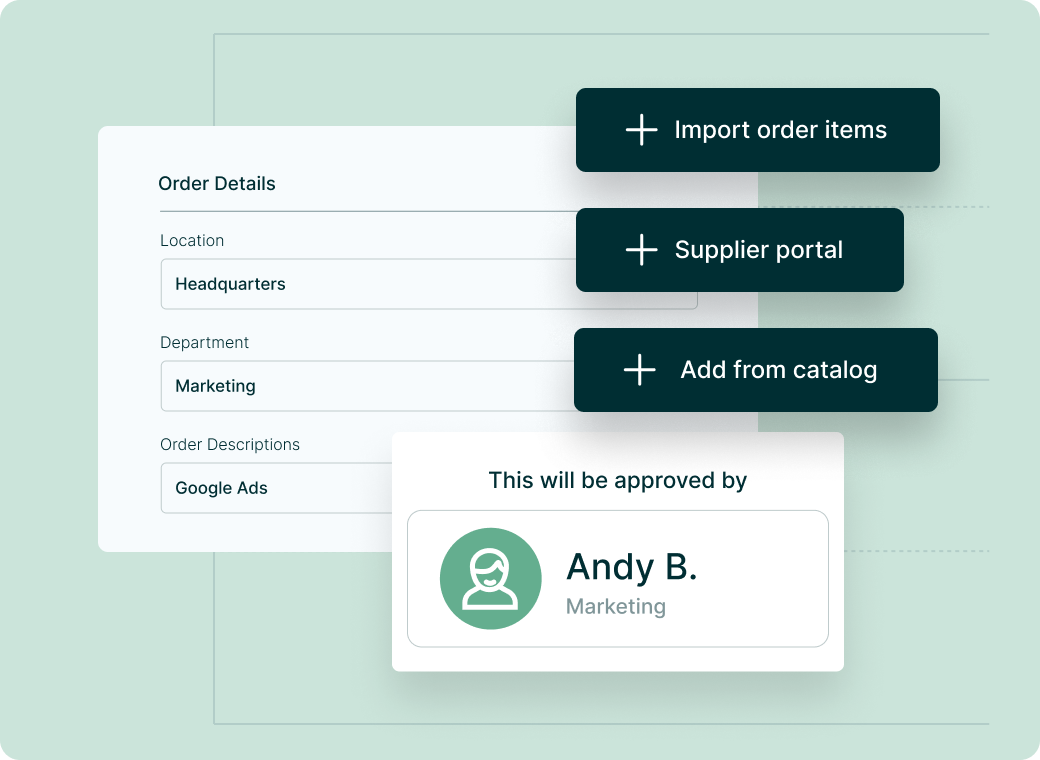
Track and analyze every stage of your purchasing journey with Procurify: easily request purchases, notify approvers, build purchase orders, receive items, and reconcile payments.
-
Designate purchasing permissions and personalize how you manage workflows
-
Consolidate orders for specific vendors and adjust as needed
-
Conduct three-way matches and confidently pay invoices from Procurify
-
Integrate with your accounting system and ERP to ensure data flows where it needs to
Real-time budget tracking
Manage all budgets in real time, from one unified platform. See how much budget you’ve already spent and know exactly what’s left before approving the next request.
-
Set up budgets based on programs, locations, projects, and more
-
See how purchases impact a specific budget before approving
-
Review real-time graphs that show actual over-committed spending
-
Stop waiting for month end to see how much your team has spent
Flexible user permissions
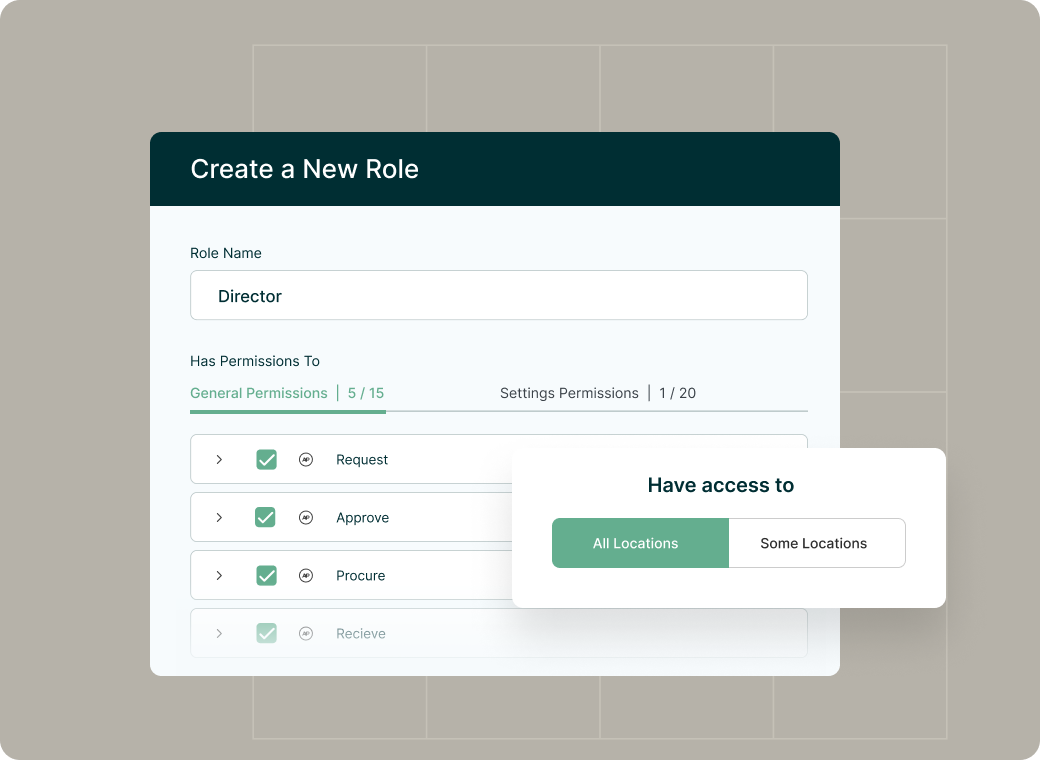
Increase control, retain compliance, and improve flexibility with quick and easy user access management.
-
Set granular access to specific modules and data categories
-
Set unique user permissions and configure approval routing according to your needs
-
Secure sensitive data and reduce your risk of data breaches
Learn what our customers have to say
Discover how healthcare organizations are leveraging Procurify to unlock efficiency improvements that free up time to focus on their patients and research.


